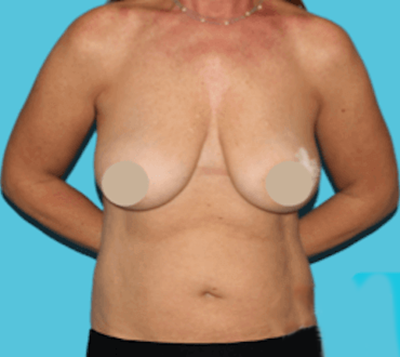
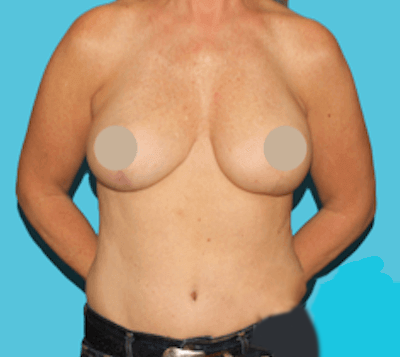
Breast Reconstruction Options
There are a number of techniques used for breast reconstruction, and our surgeons custom-tailor each treatment plan to suit a patient’s unique needs and desires.2
Deep Inferior Epigastric Perforator (DIEP) Flap Breast Reconstruction
In most cases, DIEP flap breast reconstruction is our breast reconstruction procedure of choice, as it allows our patients to enjoy restored confidence with reconstructed breasts that look and feel natural. With a DIEP flap procedure, breasts are reconstructed using skin and fat from the patient’s lower abdominal area without the need to cut or remove any muscle, which reduces recovery time and discomfort.
Stacked Deep Inferior Epigastric Perforator (DIEP) Flap Breast Reconstruction
In some cases, patients may not have adequate fat and skin in the lower abdominal area to be used in breast reconstruction. For these patients, we are able to achieve fantastic results by combining two separate flaps to reconstruct a single breast with what is known as Stacked DIEP flap breast reconstruction. These flaps may be from the inner thigh (PAP flap), from the abdomen (DIEP flap), or a combination of both.
Superficial Inferior Epigastric Artery (SIEA) Flap Breast Reconstruction
SIEA flap breast reconstruction is very similar to DIEP flap breast reconstruction in that it is also a muscle-sparing procedure during which skin, fat, and blood vessels are harvested from the abdomen. This type of breast reconstruction utilizes a different section of blood vessels from those used in DIEP flap reconstruction, which are smaller and more superficial. As a result, not all patients are ideal candidates for SIEA flap breast reconstruction.
Profunda Artery Perforator (PAP) Flap Breast Reconstruction
With PAP flap breast reconstruction, our Houston plastic surgeons harvest tissue and blood vessels from the inner posterior area of the patient’s thigh to build breasts that are soft, supple, and natural-looking. PAP flap breast reconstruction is an excellent option for patients who have undergone previous breast reconstruction procedures that yielded unsatisfactory results or for patients who delay breast reconstruction after mastectomy. This procedure can also be performed immediately after mastectomy.
Superior/Inferior Gluteal Artery (GAP) Flap Breast Reconstruction
GAP flap breast reconstruction uses fat, skin, and blood vessels harvested from the patient’s upper superior gluteal artery perforator (sGAP flap), lower buttock region (inferior gluteal artery perforator or iGAP flap), or both (bilateral GAP flap). Using advanced techniques, our surgeons are able to use this procedure to reconstruct one breast at a time with minimal scarring and no nerve or muscle damage to the buttocks.
Direct Implant
The above-noted breast reconstruction procedures use tissues harvested from the patient’s own body to rebuild the breasts (autologous breast reconstruction). Our Houston plastic surgeons are also highly experienced in using saline or silicone implants to reconstruct the breasts. A direct implant breast reconstruction may be the best option for patients who don’t have sufficient excess tissue to be harvested to rebuild the breasts, patients who are not good candidates for a more lengthy flap reconstruction procedure, or patients who wish to avoid incisions on other parts of their bodies. It is important to note, however, that this type of reconstruction may require multiple office visits or procedures and could yield results that look and feel less natural than an autologous breast reconstruction procedure.
Tissue Expanders
In patients whose breast reconstruction will be conducted in stages or those who have had significant skin removed during mastectomy, it may be necessary to employ tissue expanders. Tissue expanders are somewhat like balloons, and are used to create enough space to accommodate a breast implant. Over the course of a number of months, fluid will incrementally be added to tissue expanders so that the skin is gradually stretched to make room for the breast implant.
Our surgeons are skilled in all types of reconstruction, and can use either tissue and fat from the patient’s own body (abdomen, thigh, buttocks, etc.) or silicone/saline implants. The technique depends on the patient, but our doctors will discuss your options with you during an initial consultation.